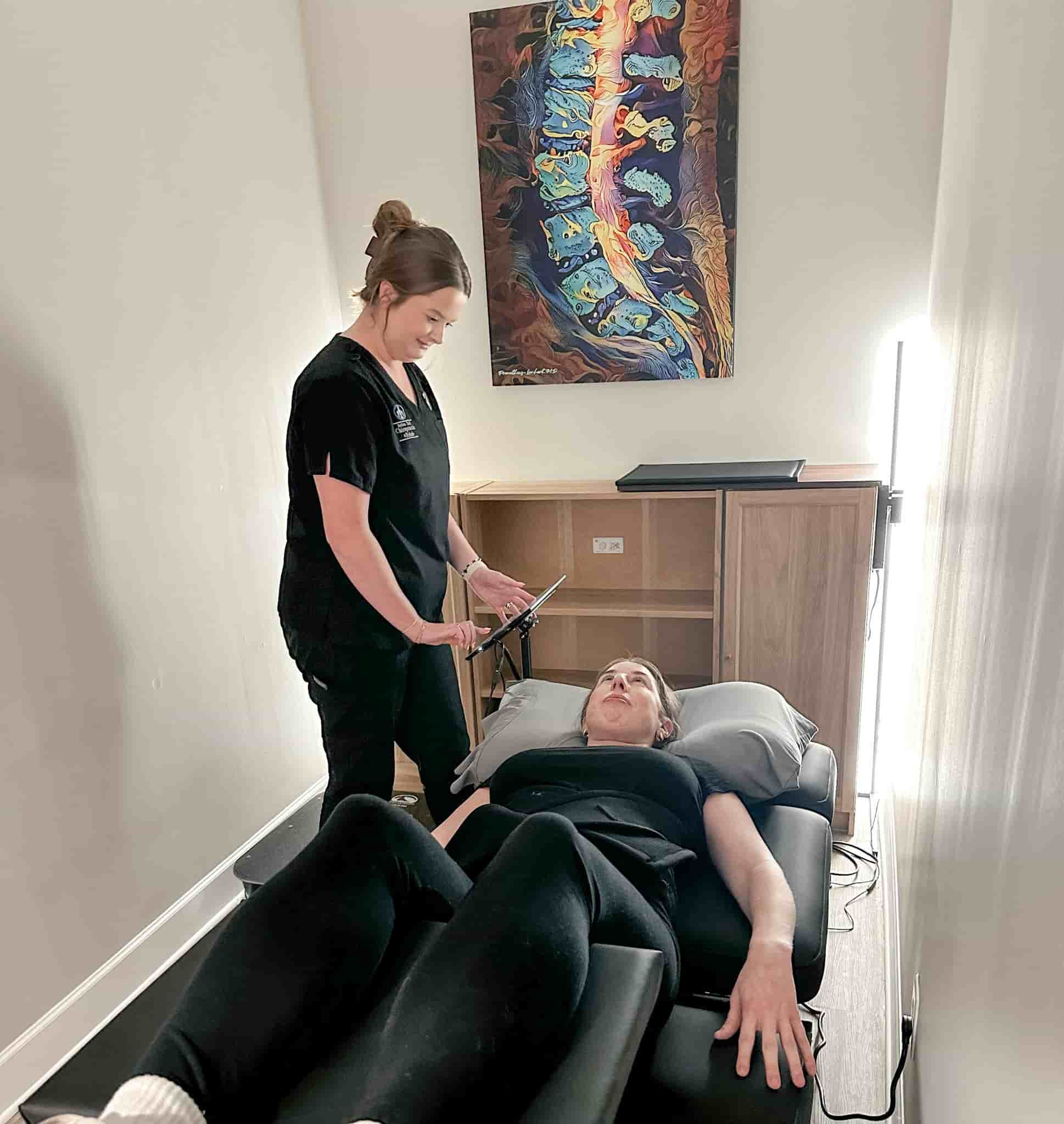
If you’ve been dealing with chronic back pain, sciatica, or a herniated disc, you’ve probably heard the term “spinal decompression” thrown around. Here’s the straightforward answer: spinal decompression is a non-surgical treatment that gently stretches the spine to reduce pressure on compressed discs and nerves. It produces strong results for disc-related conditions specifically, and for patients who qualify, it’s one of the most effective conservative options available before considering surgery.
What Actually Happens During Spinal Decompression
Spinal decompression uses a specialized table to create controlled, measured stretching of the spine. You lie down, get secured with a harness system, and the table applies gentle pulling forces to specific areas of your spine. The treatment alternates between stretch and relaxation phases, which creates a pumping action inside the disc.
That pumping matters more than you might think. When a disc is compressed all day – which happens just from standing, sitting, and moving around – fluid and nutrients get squeezed out. Decompression creates negative pressure inside the disc space, which allows oxygen, water, and healing nutrients to flow back in. It also pulls bulging disc material away from pinched nerves.
Each session typically lasts 20 to 30 minutes. Most patients describe it as surprisingly comfortable – some even fall asleep during treatment.
How It’s Different From Hanging Upside Down or Using an Inversion Table

Fair question. If decompression is just stretching the spine, can’t you get the same effect from an inversion table in your garage?
Not quite. Inversion tables apply gravitational force, which does create some spinal stretch. But it’s uncontrolled and non-specific. You’re stretching everything at once, and your body’s natural response is often to tighten up and resist the pull. That muscle guarding works directly against what you’re trying to accomplish.
Professional spinal decompression uses computerized force calibrated to your body weight and condition. The table targets specific spinal segments – say, the L4-L5 disc – without loading the entire spine. And because the force ramps up gradually and alternates with relaxation, your muscles don’t contract defensively. The treatment bypasses that protective reflex, which is the whole point.
Plus, hanging upside down increases pressure in your eyes and head, which isn’t ideal for most people. Decompression tables keep you horizontal – no blood-rushing-to-your-head situation.
Who Benefits Most From Spinal Decompression
Decompression works best for nerve-related pain caused by disc problems. That includes herniated discs, bulging discs, degenerative disc disease, and sciatica stemming from disc compression. If your pain shoots down your leg, causes numbness or tingling, or gets worse when you sit or bend forward, you’re likely dealing with a disc issue – and decompression is well-suited for that presentation.
We also see strong results with patients who have posterior facet syndrome and certain cases of spinal stenosis, where the spinal canal has narrowed and is compressing nerves.
The treatment is particularly effective for people who’ve already tried physical therapy, medication, and rest without meaningful improvement. These are patients stuck in that frustrating middle zone – too much pain to ignore, but not severe enough to justify surgery. Decompression is often exactly what moves the needle for them.
At Indian Trail Chiropractic & Rehab, Dr. Gentile evaluates whether decompression fits your specific case. Not everyone with back pain needs it, and not everyone with a disc issue is a good candidate. But when it’s the right fit, the results are significant.
Who Shouldn’t Use Spinal Decompression
Decompression isn’t appropriate for everyone, and any honest provider will tell you that upfront. You’re not a candidate if you’re pregnant, have severe osteoporosis, or have had spinal fusion surgery in the area being treated. The forces involved could cause harm in those situations.
If you have a tumor, fracture, or infection in your spine, decompression is off the table entirely. Same goes for severe nerve damage or advanced cases where conservative care has clearly run its course and surgery is the appropriate next step.
Age alone doesn’t disqualify you – we’ve treated patients in their 70s successfully – but overall bone health and spinal stability matter. Dr. Gentile reviews imaging and medical history before recommending decompression. If it’s not the right approach, he’ll tell you directly and explain what is.
What to Expect During Treatment
Spinal decompression isn’t a one-and-done treatment. Disc healing takes time – you’re dealing with tissue that has poor blood supply and constant mechanical stress throughout the day. The evaluation determines how many sessions are appropriate based on your specific condition, how long it’s been present, and how your body responds.
Some patients feel relief after the first few sessions. Others take a couple of weeks to notice significant change. We reassess regularly and adjust the protocol based on how you’re progressing.
The goal isn’t just short-term pain relief. We’re working toward lasting structural change – getting disc material to retract, reducing inflammation around the nerve, and restoring normal movement patterns. That requires consistency on your end as well as ours.
Decompression consistently produces its best results when combined with other treatments. At our practice, we pair it with chiropractic adjustments, corrective exercises, and when indicated, soft tissue work like Active Release Technique. Decompression reduces pressure on the disc, adjustments restore proper joint alignment, and exercises retrain your movement patterns so the problem doesn’t come right back.
The Real Question: Is It Worth Trying?
If you’re living with daily pain that limits what you can do – whether that’s playing with your kids, working without constant discomfort, or just getting through the day without wincing every time you bend over – decompression is worth a serious look.
It’s non-invasive, has minimal risk, and doesn’t burn any bridges. For patients dealing with sciatica, herniated discs, or chronic low back pain that hasn’t responded to other treatments, decompression delivers real, lasting relief without the downtime and risks of surgery.
The key is an accurate diagnosis first. Not all back pain comes from discs, and decompression won’t help if the problem is muscular, ligament-related, or caused by something like a hip issue referring pain into your back. That’s exactly what the evaluation is designed to sort out.
Dr. Gentile has treated thousands of patients with disc-related pain over his 20+ years in practice. If decompression makes sense for your situation, he’ll explain why. If it doesn’t, he’ll tell you what does.
FAQs
Does spinal decompression hurt?
No. Most patients find it comfortable and relaxing. You’ll feel a gentle pulling sensation, but it shouldn’t cause pain. If you do feel discomfort, the treatment is adjusted immediately.
How long do results last?
That depends on your condition and what you do after treatment. Patients who follow through with corrective exercises and maintain good movement habits consistently hold their results well. Others may benefit from occasional maintenance sessions down the road.
Will insurance cover spinal decompression?
Coverage varies. Some plans cover it under chiropractic care, while others don’t. We can verify your benefits and discuss payment options when you come in.
Can decompression fix a herniated disc completely?
In many cases, yes – imaging has shown disc material retracting after a full course of treatment. And even when the disc doesn’t fully remodel, reducing pressure on the nerve eliminates symptoms for most patients. That’s what matters most for getting your life back.
Ready to find out if spinal decompression is right for you? Schedule an appointment with Dr. Gentile or call (704) 821-3222.

